Table of Contents
- Introduction to Gynecomastia
- What General Anesthesia Actually Means
- Understanding Male Breast Reduction
- Our Approach: Local Anesthesia with Physiologic Stability
- Surgical Options for Gynecomastia
- Faster Recovery, Lower Systemic Burden
- The GLP-1 Era: A New Relevance
- Addressing Patient Anxiety
- When General Anesthesia Is Appropriate
- Precision Over Theater
- The Broader Philosophy
- Preparation and Recovery from Breast Reduction Surgery
- Efficiency Without Compromise
- Conclusion: Refinement, Not Reduction
Using general anesthesia in this setting often adds systemic risk without adding meaningful surgical benefit.Gynecomastia surgeon, Dr. Edwin Ishoo states, “This is a confined area. In my opinion, general anesthesia is completely unwarranted for 99% of patients.” That statement reflects years of surgical experience and outcomes.Puffy nipples are a common concern for many men with gynecomastia, and this can be addressed during surgery. During your consultation, you will discuss your concerns about your chest contour, go over your options for male breast reduction surgery, and have the opportunity to ask any questions you may have about your procedure.
Introduction to Gynecomastia
Gynecomastia is a common condition in which men develop excess breast tissue in the chest area, resulting in the appearance of enlarged breasts. This can occur due to a variety of factors, including hormonal changes, genetics, obesity, and the use of certain drugs. The presence of excess breast tissue, excess skin, and excess fat can cause significant emotional distress and impact self confidence, as many men feel uncomfortable with the appearance of their chest. For patients struggling with gynecomastia, male breast reduction and breast reduction surgery offer effective treatment options. A skilled plastic surgeon can assess the underlying cause and recommend the most appropriate surgical plan to remove unwanted tissue and restore a more masculine appearance. By addressing the physical and emotional effects of gynecomastia, surgery can help patients regain confidence and feel more comfortable in their own bodies.
What General Anesthesia Actually Means
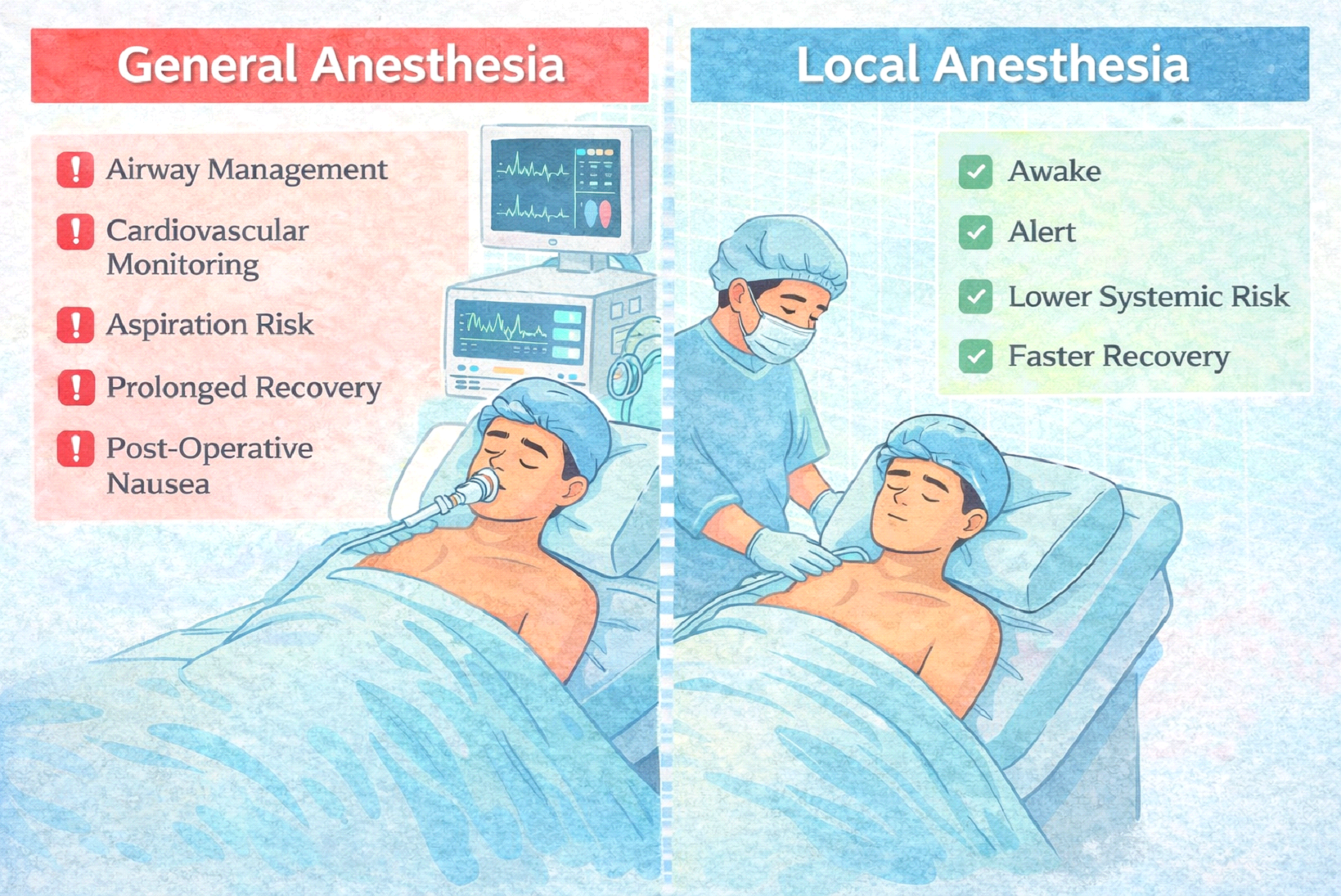
Under general anesthesia, patients are intubated or deeply sedated. Airway management becomes part of the procedure. Cardiovascular monitoring becomes more complex. Nausea and post-operative grogginess become more likely.In healthy individuals, the absolute risk is low. But low is not zero.There are:
- Airway considerations • Cardiovascular fluctuations • Aspiration risk • Prolonged recovery monitoring • Post-operative nausea • Delayed return to normal activity
Understanding Male Breast Reduction
Male breast reduction, also known as gynecomastia surgery, is a plastic surgery procedure designed to remove excess breast tissue, fat, and skin from the male chest. The goal of this surgical procedure is to create flatter, firmer chest contours and restore a more masculine appearance. For many men, gynecomastia leads to physical changes that can affect self confidence and quality of life. Male breast reduction surgery is often described as life changing, as it allows patients to feel more comfortable in their own skin and wear clothing with confidence. The procedure may involve liposuction to remove excess fat, as well as direct excision of glandular tissue and skin to achieve optimal results. After surgery, patients typically wear a compression garment to support the surrounding tissues, minimize swelling, and promote a faster recovery. With the help of an experienced plastic surgeon, most patients experience a significant improvement in both their physical appearance and self esteem.
Our Approach: Local Anesthesia with Physiologic Stability
At Regeneris, gynecomastia surgery is performed under local anesthesia with supportive oral medications.Patients receive carefully selected medications that reduce nausea, blunt mild anxiety, and promote comfort. Some may drift into a light sleep. They are not intubated. They are not deeply sedated. They remain physiologically stable throughout the procedure. patients “may fall asleep lightly, but they wake up immediately and are alert.” The difference is visible.There is no disorientation. No prolonged grogginess. No need for extended recovery monitoring. Most patients are walking out within a short period of time, clear-headed and stable. This is not bravado. It is surgical discipline.
Surgical Options for Gynecomastia
There are several surgical options available for treating gynecomastia, and the best approach depends on the severity of the condition and the patient’s unique anatomy. A skilled plastic surgeon will develop a customized surgical plan that may include liposuction to remove excess fat, surgical excision to address glandular tissue, or a combination of both techniques. In cases where there is significant excess skin or glandular tissue, larger incisions may be required to achieve the desired chest contours and a natural, masculine appearance. For patients with less severe gynecomastia, smaller incisions and less invasive techniques may be sufficient. The surgeon will consider factors such as muscle mass, the amount of excess skin and fat, and the overall shape of the chest when recommending surgical options. The primary goal is to achieve a smooth, masculine chest with minimal scarring and a faster recovery process, allowing patients to return to their normal activities with renewed confidence.
Faster Recovery, Lower Systemic Burden
The best erectile dysfunction treatment depends on individual circumstances, health status, and treatment goals. Viagra and oral medications make excellent choices for men who:
- Want immediate results for occasional ED
- Have contraindications to shockwave therapy
- Prefer the simplicity of taking a pill
- Can’t commit to multiple treatment sessions
- Have ED primarily from psychological rather than vascular causes
- Desire lasting results without ongoing medication
- Have a vascular-based ED with adequate remaining blood flow
- Want to address the underlying cause of their condition
- Are willing to invest in upfront treatment costs
- Seek a drug-free approach to sexual health
The GLP-1 Era: A New Relevance
This approach has become even more relevant in the era of GLP-1 medications such as semaglutide and tirzepatide. These medications slow gastric emptying. Anesthesiologists increasingly screen for GLP-1 use before elective procedures because of aspiration concerns under general anesthesia. Some procedures are postponed. Others require extended fasting protocols.With local anesthesia, that issue is largely bypassed. Dr. Ishoo notes “Many GLP-1 patients are contraindicated for general anesthesia, so our local approach is beneficial.”Weight loss medications are transforming body composition. As fat diminishes, glandular gynecomastia often becomes more visible. These patients deserve a safe, efficient path to definitive gland removal without introducing new systemic concerns. Local anesthesia provides that path.
Addressing Patient Anxiety
Patients often ask:
- Will I feel pain?
- Will I hear everything?
- Will I be uncomfortable?
- What if I do not wake up?
- What if I wake up nauseated?
- What if I feel disoriented?
When General Anesthesia Is Appropriate
Local anesthesia is not dogma. It is judgment.There are cases where hospital-based anesthesia is appropriate:
- Severe procedural anxiety • Complex medical comorbidities • Unusual anatomical considerations • Combined multi-procedure operations • Complex cases, such as revision surgeries or challenging anatomical scenarios • Severe cases of gynecomastia with significant excess tissue and skin
Precision Over Theater
There is a cultural assumption that bigger anesthesia equals more serious surgery. That assumption is misleading.Gynecomastia surgery requires:
- Complete gland removal • Strategic liposuction • Sculpted chest contour • Attention to the lateral border • Definition of the inferior pectoral line
The Broader Philosophy
Aesthetic surgery, at its best, is disciplined medicine. It is not spectacle.The male chest is a visible anatomical structure tied to posture, confidence, and identity. Correcting glandular enlargement restores contour. It should not simultaneously burden the cardiovascular and respiratory systems unnecessarily.The concept is simple:Minimize risk.
Maximize precision.
Deliver durable results.Local anesthesia allows us to do exactly that.
Preparation and Recovery from Breast Reduction Surgery
Preparing for male breast reduction surgery begins with a comprehensive medical history review, including an assessment of hormonal changes and any drug use that may contribute to gynecomastia. Identifying the underlying cause is essential for planning the most effective treatment. Patients are typically advised to discontinue certain medications, such as blood thinners, and to avoid strenuous activity in the days leading up to surgery. After the procedure, a compression vest is worn to support the chest area, reduce swelling, and aid in the healing process. The recovery process usually takes about two weeks, during which patients should avoid heavy lifting and strenuous activity to ensure proper healing. Pain is generally well managed with medication, and most patients can expect to see their final results within a few months. Attending all follow-up appointments and closely following the surgeon’s instructions are key to achieving the best possible outcome. With proper preparation and care, breast reduction surgery can be a life changing experience, helping men achieve a more masculine appearance and improved self confidence.
Efficiency Without Compromise
Most procedures take one to two hours. Patients return home the same day. There is no prolonged observation. No hospital stay. No intubation recovery.They begin healing immediately in their own environment.Post-operative care — compression, massage, activity modification — becomes the focus; post-op management determines a substantial portion of the final outcome.The surgery is one component. Recovery discipline is the other. Local anesthesia keeps that entire arc efficient and controlled.
Conclusion: Refinement, Not Reduction
Gynecomastia surgery does not require full, systemic anesthesia. It requires precision. In the right patient, local anesthesia reduces systemic exposure, accelerates recovery, lowers cost, and maintains surgical excellence. We do not avoid general anesthesia out of ideology. We avoid it when it does not add value.In a confined anatomical correction such as male breast reduction, adding systemic suppression of consciousness often increases burden without improving result. For most men, local anesthesia is not a lesser option. It is the better one.
Peak Masculinity
Starts Here

By Dr. Ryan Welter
February 19, 2026
Using general anesthesia in this setting often adds systemic risk without adding meaningful surgical benefit.Gynecomastia surgeon, Dr. Edwin Ishoo states, “This is a confined area. In my opinion, general anesthesia is completely unwarranted for 99% of patients.” That statement reflects years of surgical experience and outcomes.Puffy nipples are a common concern for many men with gynecomastia, and this can be addressed during surgery. During your consultation, you will discuss your concerns about your chest contour, go over your options for male breast reduction surgery, and have the opportunity to ask any questions you may have about your procedure.
Introduction to Gynecomastia
Gynecomastia is a common condition in which men develop excess breast tissue in the chest area, resulting in the appearance of enlarged breasts. This can occur due to a variety of factors, including hormonal changes, genetics, obesity, and the use of certain drugs. The presence of excess breast tissue, excess skin, and excess fat can cause significant emotional distress and impact self confidence, as many men feel uncomfortable with the appearance of their chest. For patients struggling with gynecomastia, male breast reduction and breast reduction surgery offer effective treatment options. A skilled plastic surgeon can assess the underlying cause and recommend the most appropriate surgical plan to remove unwanted tissue and restore a more masculine appearance. By addressing the physical and emotional effects of gynecomastia, surgery can help patients regain confidence and feel more comfortable in their own bodies.
What General Anesthesia Actually Means
Under general anesthesia, patients are intubated or deeply sedated. Airway management becomes part of the procedure. Cardiovascular monitoring becomes more complex. Nausea and post-operative grogginess become more likely.In healthy individuals, the absolute risk is low. But low is not zero.There are:
- Airway considerations • Cardiovascular fluctuations • Aspiration risk • Prolonged recovery monitoring • Post-operative nausea • Delayed return to normal activity
Understanding Male Breast Reduction
Male breast reduction, also known as gynecomastia surgery, is a plastic surgery procedure designed to remove excess breast tissue, fat, and skin from the male chest. The goal of this surgical procedure is to create flatter, firmer chest contours and restore a more masculine appearance. For many men, gynecomastia leads to physical changes that can affect self confidence and quality of life. Male breast reduction surgery is often described as life changing, as it allows patients to feel more comfortable in their own skin and wear clothing with confidence. The procedure may involve liposuction to remove excess fat, as well as direct excision of glandular tissue and skin to achieve optimal results. After surgery, patients typically wear a compression garment to support the surrounding tissues, minimize swelling, and promote a faster recovery. With the help of an experienced plastic surgeon, most patients experience a significant improvement in both their physical appearance and self esteem.
Our Approach: Local Anesthesia with Physiologic Stability
At Regeneris, gynecomastia surgery is performed under local anesthesia with supportive oral medications.Patients receive carefully selected medications that reduce nausea, blunt mild anxiety, and promote comfort. Some may drift into a light sleep. They are not intubated. They are not deeply sedated. They remain physiologically stable throughout the procedure. patients “may fall asleep lightly, but they wake up immediately and are alert.” The difference is visible.There is no disorientation. No prolonged grogginess. No need for extended recovery monitoring. Most patients are walking out within a short period of time, clear-headed and stable. This is not bravado. It is surgical discipline.
Surgical Options for Gynecomastia
There are several surgical options available for treating gynecomastia, and the best approach depends on the severity of the condition and the patient’s unique anatomy. A skilled plastic surgeon will develop a customized surgical plan that may include liposuction to remove excess fat, surgical excision to address glandular tissue, or a combination of both techniques. In cases where there is significant excess skin or glandular tissue, larger incisions may be required to achieve the desired chest contours and a natural, masculine appearance. For patients with less severe gynecomastia, smaller incisions and less invasive techniques may be sufficient. The surgeon will consider factors such as muscle mass, the amount of excess skin and fat, and the overall shape of the chest when recommending surgical options. The primary goal is to achieve a smooth, masculine chest with minimal scarring and a faster recovery process, allowing patients to return to their normal activities with renewed confidence.
Faster Recovery, Lower Systemic Burden
The best erectile dysfunction treatment depends on individual circumstances, health status, and treatment goals. Viagra and oral medications make excellent choices for men who:
- Want immediate results for occasional ED
- Have contraindications to shockwave therapy
- Prefer the simplicity of taking a pill
- Can’t commit to multiple treatment sessions
- Have ED primarily from psychological rather than vascular causes
- Desire lasting results without ongoing medication
- Have a vascular-based ED with adequate remaining blood flow
- Want to address the underlying cause of their condition
- Are willing to invest in upfront treatment costs
- Seek a drug-free approach to sexual health
The GLP-1 Era: A New Relevance
This approach has become even more relevant in the era of GLP-1 medications such as semaglutide and tirzepatide. These medications slow gastric emptying. Anesthesiologists increasingly screen for GLP-1 use before elective procedures because of aspiration concerns under general anesthesia. Some procedures are postponed. Others require extended fasting protocols.With local anesthesia, that issue is largely bypassed. Dr. Ishoo notes “Many GLP-1 patients are contraindicated for general anesthesia, so our local approach is beneficial.”Weight loss medications are transforming body composition. As fat diminishes, glandular gynecomastia often becomes more visible. These patients deserve a safe, efficient path to definitive gland removal without introducing new systemic concerns. Local anesthesia provides that path.
Addressing Patient Anxiety
Patients often ask:
- Will I feel pain?
- Will I hear everything?
- Will I be uncomfortable?
- What if I do not wake up?
- What if I wake up nauseated?
- What if I feel disoriented?
When General Anesthesia Is Appropriate
Local anesthesia is not dogma. It is judgment.There are cases where hospital-based anesthesia is appropriate:
- Severe procedural anxiety • Complex medical comorbidities • Unusual anatomical considerations • Combined multi-procedure operations • Complex cases, such as revision surgeries or challenging anatomical scenarios • Severe cases of gynecomastia with significant excess tissue and skin
Precision Over Theater
There is a cultural assumption that bigger anesthesia equals more serious surgery. That assumption is misleading.Gynecomastia surgery requires:
- Complete gland removal • Strategic liposuction • Sculpted chest contour • Attention to the lateral border • Definition of the inferior pectoral line
The Broader Philosophy
Aesthetic surgery, at its best, is disciplined medicine. It is not spectacle.The male chest is a visible anatomical structure tied to posture, confidence, and identity. Correcting glandular enlargement restores contour. It should not simultaneously burden the cardiovascular and respiratory systems unnecessarily.The concept is simple:Minimize risk.
Maximize precision.
Deliver durable results.Local anesthesia allows us to do exactly that.
Preparation and Recovery from Breast Reduction Surgery
Preparing for male breast reduction surgery begins with a comprehensive medical history review, including an assessment of hormonal changes and any drug use that may contribute to gynecomastia. Identifying the underlying cause is essential for planning the most effective treatment. Patients are typically advised to discontinue certain medications, such as blood thinners, and to avoid strenuous activity in the days leading up to surgery. After the procedure, a compression vest is worn to support the chest area, reduce swelling, and aid in the healing process. The recovery process usually takes about two weeks, during which patients should avoid heavy lifting and strenuous activity to ensure proper healing. Pain is generally well managed with medication, and most patients can expect to see their final results within a few months. Attending all follow-up appointments and closely following the surgeon’s instructions are key to achieving the best possible outcome. With proper preparation and care, breast reduction surgery can be a life changing experience, helping men achieve a more masculine appearance and improved self confidence.
Efficiency Without Compromise
Most procedures take one to two hours. Patients return home the same day. There is no prolonged observation. No hospital stay. No intubation recovery.They begin healing immediately in their own environment.Post-operative care — compression, massage, activity modification — becomes the focus; post-op management determines a substantial portion of the final outcome.The surgery is one component. Recovery discipline is the other. Local anesthesia keeps that entire arc efficient and controlled.
Conclusion: Refinement, Not Reduction
Gynecomastia surgery does not require full, systemic anesthesia. It requires precision. In the right patient, local anesthesia reduces systemic exposure, accelerates recovery, lowers cost, and maintains surgical excellence. We do not avoid general anesthesia out of ideology. We avoid it when it does not add value.In a confined anatomical correction such as male breast reduction, adding systemic suppression of consciousness often increases burden without improving result. For most men, local anesthesia is not a lesser option. It is the better one.
Peak Masculinity
Starts Here

By Dr. Ryan Welter
February 19, 2026




