- Introduction to Gynecomastia
- Causes and Risk Factors
- The Anatomy of Getting It Wrong
- Why Vision Matters in Human Identity
- Recurrence: The Long-Term Consequence of Incomplete Gynecomastia Surgery
- The Technical Philosophy of Male Breast Reduction at Regeneris
- Potential Risks and Complications
- Recovery and Aftercare
- The Personal Dimension
- A Thoughtful Conclusion
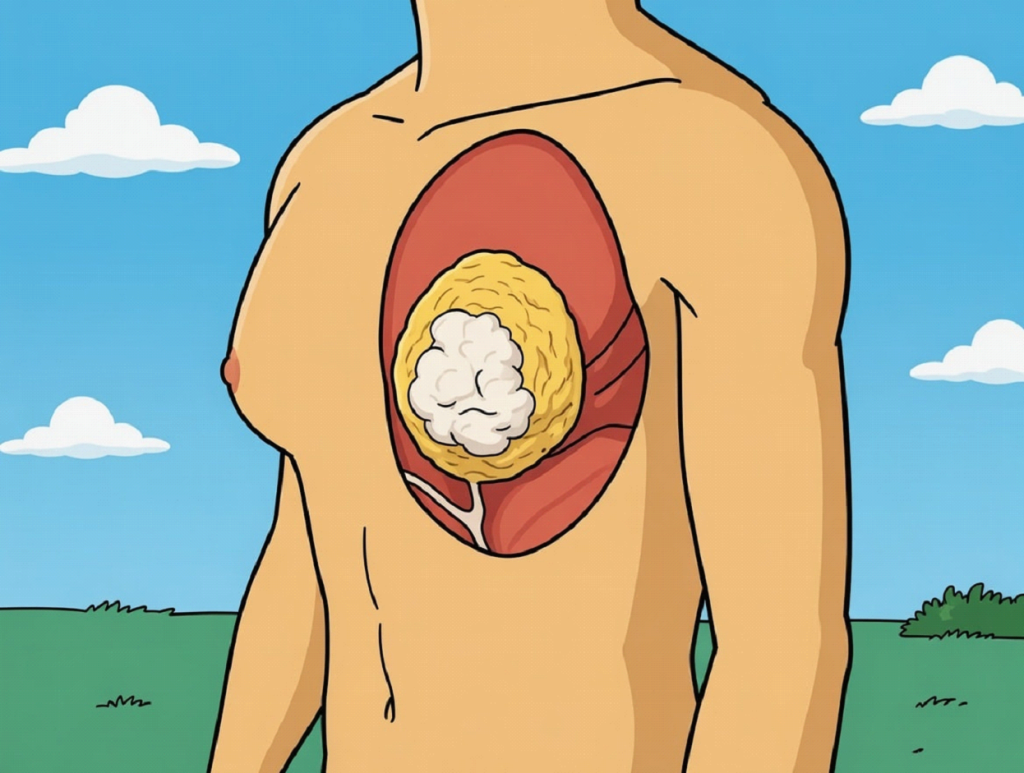
Introduction to Gynecomastia
Causes and Risk Factors
The Anatomy of Getting It Wrong
- Complete gland excision • Strategic liposuction • Sculpted contouring of the lateral and inferior chest borders
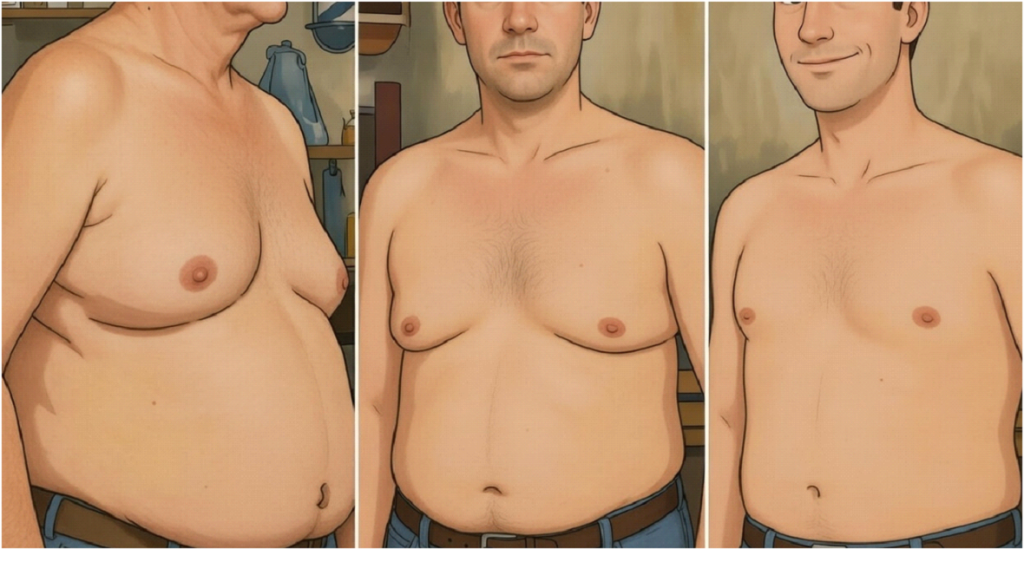
Why Vision Matters in Human Identity
Recurrence: The Long-Term Consequence of Incomplete Gynecomastia Surgery
The Technical Philosophy of Male Breast Reduction at Regeneris
- The ratio of gland to fat • Skin elasticity and turgor • The patient’s age and hormonal status • Lifestyle factors including testosterone therapy • Athletic goals and downtime tolerance
Potential Risks and Complications
Recovery and Aftercare
The Personal Dimension
- The teenage athlete who avoided the pool • The executive who never felt comfortable in fitted clothing • The man who lost fifty pounds and still avoids taking his shirt off • The husband who wants to feel confident in intimacy

A Thoughtful Conclusion
Gynecomastia is common, especially during adolescence due to hormone changes, and in many cases observation may lead to spontaneous resolution. However, the way it is treated should not be casual. Certain drugs can contribute to the development of gynecomastia by affecting hormone levels. Liposuction alone is insufficient when gland is present. Partial excision invites recurrence. Over-aggressive resection invites deformity.
Comprehensive, anatomically informed surgery produces stable results. Medication to balance hormones is most effective during the early, active phase of gynecomastia, but its effectiveness diminishes as the tissue becomes permanently fibrotic. We do not approach gynecomastia as a trend procedure. We approach it as an anatomical correction rooted in physiology and informed by the deeper realities of human identity.
The human body did not evolve casually. It reflects energy investment, structure, and signaling. When that structure is disrupted by glandular enlargement, restoring it thoughtfully is not superficial. It is precise medicine applied to visible anatomy.
Preoperative evaluation for gynecomastia should include screening for breast cancer and male breast cancer to ensure comprehensive care. At Regeneris, we believe in doing it once, doing it thoroughly, and doing it with respect for both the technical and human dimensions of the male chest.
Gynecomastia surgery done right is not about flattening tissue. It is about restoring definition — and with it, confidence that does not require explanation.
Peak Masculinity
Starts Here

By Dr. Ryan Welter
February 19, 2026




