- Gynecomastia (Excess Male Breast Tissue) Is Not a Fitness Problem
- Common Causes in Adult Men
- Why Diet and Exercise Do Not Fix It
- Surgical vs Non-Surgical Options
- Types of Gynecomastia Surgery
- Recovery Timeline
- Cost of Gynecomastia Surgery in Boston
- Choosing a Qualified Gynecomastia Surgeon
- Why Men Choose Regeneris Men
- Frequently Asked Questions
- Final Thoughts
Gynecomastia (Excess Male Breast Tissue) Is Not a Fitness Problem
Gynecomastia is the benign enlargement of male breast tissue. It is not the same thing as chest fat. True gynecomastia involves glandular tissue beneath the nipple-areolar complex, often mixed with some fat.
Medically, it reflects an imbalance between estrogenic and androgenic activity at the tissue level. Estrogen does not need to be high for this to occur. A relative drop in androgen effect is enough.
Cosmetically, gynecomastia alters the male chest contour in ways that are difficult to hide:
- Rounded or protruding nipples
- Persistent fullness despite low body fat
- Asymmetry between sides
- Self-consciousness in fitted clothing or at the gym
Once established in adult men, glandular tissue rarely regresses on its own.

Common Causes in Adult Men
- Spironolactone
- Finasteride
- Certain antidepressants and antipsychotics
- Some cardiac and blood pressure medications
Why Diet and Exercise Do Not Fix It
Surgical vs Non-Surgical Options
Types of Gynecomastia Surgery
The surgical plan depends on tissue type, skin quality, and severity.
Glandular excision
Dense glandular tissue beneath the nipple is removed directly, usually through a small incision at the edge of the areola. This allows precise contouring.
Liposuction
Liposuction addresses surrounding fat and smooths transitions across the chest. It is commonly combined with excision.
Skin tightening or excision
In more advanced cases with lax skin, additional skin management may be required. This is less common but sometimes necessary.
The goal is a natural male chest contour, not simply tissue removal. Overcorrection can cause deformities. Undercorrection leads to persistence. Judgment matters.
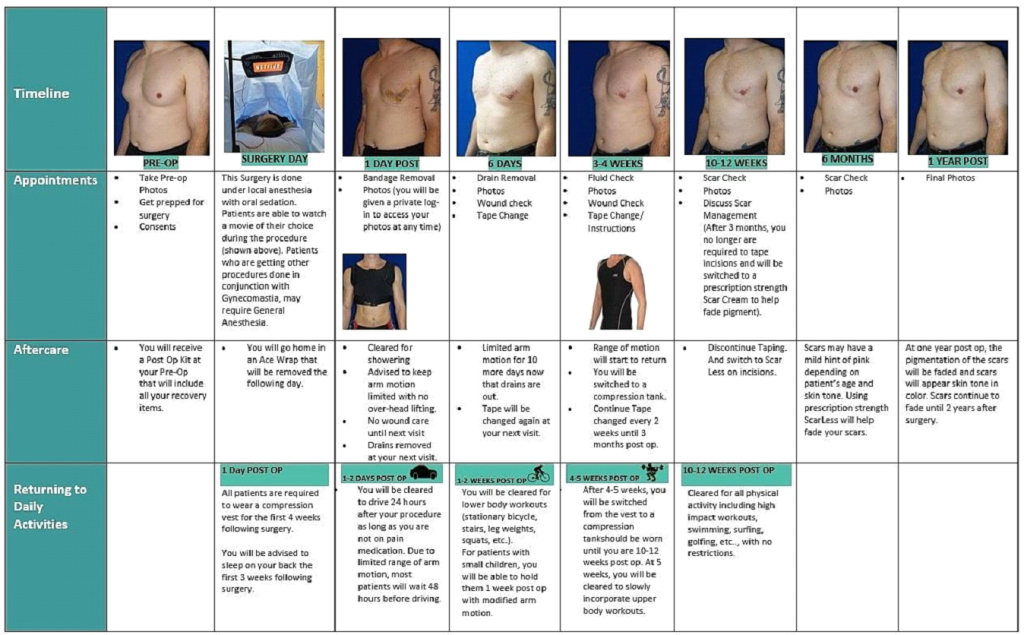
Recovery Timeline

Weeks 2 to 4
Return to desk work is common. Light activity resumes. The chest begins to look more natural, though firmness can persist.
Weeks 6 to 12
Full exercise is typically allowed. Most swelling has resolved. Early results are visible.
3 to 6 months
Final contour emerges as residual swelling subsides and tissues settle.
Cost of Gynecomastia Surgery in Boston
Choosing a Qualified Gynecomastia Surgeon
- Specific experience with male chest surgery
- Consistent before-and-after results in men
- Conservative, anatomically informed technique
- Willingness to discuss risks and limitations clearly
Why Men Choose Regeneris Men
Frequently Asked Questions
Final Thoughts
Peak Masculinity
Starts Here

By Dr. Ryan Welter
February 19, 2026




